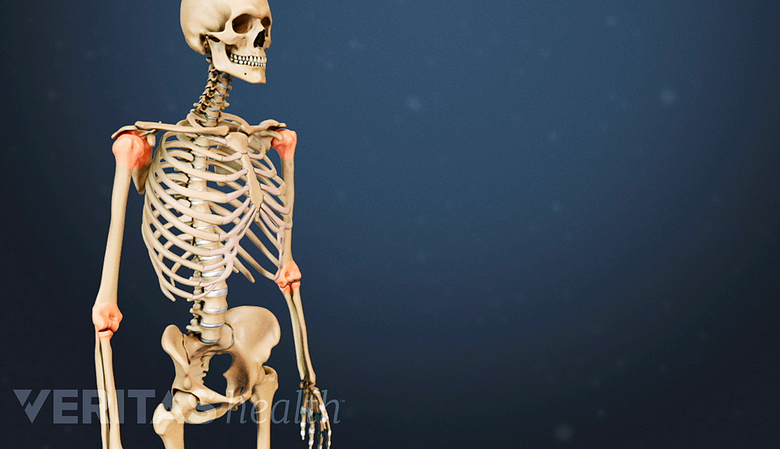
Rheumatoid arthritis (RA) is a chronic autoimmune disease that causes the immune system to attack the body’s own tissues, particularly the delicate tissue that surround joints.
RA can affect almost any joint in the body. The first signs and symptoms usually show up in the wrists, knuckles, balls of the feet, and/or knees. In addition to causing painful joint swelling and stiffness, rheumatoid arthritis can cause fever and fatigue.
Over time, RA may lead to long-term joint deformities—especially if it goes untreated or under-treated. The best way to limit joint damage is to get diagnosed, begin a treatment plan, and make adjustments to that plan if needed.
How Does Rheumatoid Arthritis Progress Over Time?
Regardless of whether symptoms appear gradually, over several months, or rapidly, rheumatoid arthritis develops the same way. The disease progresses through these steps:
1. The synovial tissue becomes inflamed
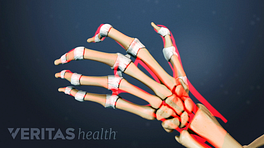
Many parts of the body, including joints, tendons, and bursae, are surrounded by a delicate membrane lining called synovial tissue (synovium). Rheumatoid arthritis causes the synovial lining surrounding a joint to become inflamed. This condition is called synovitis, and it can cause joint pain, stiffness, and swelling.
2. Pannus tissue forms
Inflammation causes the synovial tissue cells to divide and multiply, which causes the tissue to thicken, resulting in more pain and swelling. As cells continue to multiply, the tissue expands into the joint space—the space between the joint’s two bones—where it does not belong. The invading tissue is called pannus or rheumatoid pannus.
See What Is Pannus?
3. Cartilage and other joint tissues are damaged
The pannus cells release molecules called enzymes that damage cartilage and underlying bone. Over time, this damage can alter the alignment of the joints, lead to further pain and, in some cases, cause joint deformities.
Not all synovial tissue in the body will undergo these changes simultaneously. People with RA typically have certain joints that experience symptoms and other joints that do not.
In This Article:
Rheumatoid Arthritis Flare-Up
RA disease activity can get noticeably worse for a temporary period—ranging from a day to several weeks or longer. This is called a rheumatoid arthritis flare-up or RA flare. Symptoms such as stiff, painful joints and fatigue may make it difficult or impossible to get out of bed, go to work, parent, or do hobbies or basic chores.
Generally, it is a good idea to contact a physician if a flare-up lasts more than a week. A physician may want to schedule a phone call or in-office visit. He or she may also consider prescribing medications to help bring the flare under control.
RA flares can have triggers
It is possible for a specific activity or event to initiate a flare-up. The activity or event sets off inflammation in the body that is difficult to stop. A flare may be triggered by:
- An illness, such as the flu
- An injury or surgery
- Too much physical activity
- Emotional stress
- Certain foods (typically processed, fried, and/or high sugar foods)
Triggers vary from person to person. In addition, not all RA flares have clear triggers.
“Flare-up” is not an official medical term
Keep in mind that “rheumatoid arthritis flare-up” is a common term without a formal medical definition. In addition, a flare-up may not have observable, measurable signs that a doctor can recognize. For example, a flare-up may cause joint pain and fatigue without visible joint swelling or notable changes in lab test results.
See Is My Joint Pain Caused by Rheumatoid Arthritis (RA) or Another Autoimmune Disorder?
Seropositive vs. Seronegative Rheumatoid Arthritis
Physicians often distinguish between two types of rheumatoid arthritis: seropositive and seronegative. The prefix “sero” refers to blood serum. People with seropositive RA have certain protein molecules in their blood. Specifically, their blood contains either or both:
- Anti-cyclic citrullinated peptide (called anti-CCP or ACPA)
- Rheumatoid factor (RF)
Experts estimate 70% to 80% of rheumatoid arthritis are seropositive. 1 Riaz, S and Kontzias, A. Rheumatoid Arthritis. In: Efthimiou P, ed. Absolute Rheumatology Review. Springer Nature Switzerland AG; 2020; chap 15. Accessed September 15, 2020. https://doi.org/10.1007/978-3-030-23022-7_15
People who meet the diagnostic criteria for RA but have neither anti-CCP nor RF proteins in their blood are diagnosed with seronegative rheumatoid arthritis.
Seronegative RA or something else?
Occasionally, a diagnosis of seronegative RA will change. For example, if a chronic skin rash called psoriasis appears, a diagnosis of psoriatic arthritis may be considered. Similarly, if signs and symptoms appear in the spine, a diagnosis of spondyloarthritis may be considered. The treatments for these diseases are similar.
It can be helpful to recognize and track symptoms, even after a diagnosis has been made.
- 1 Riaz, S and Kontzias, A. Rheumatoid Arthritis. In: Efthimiou P, ed. Absolute Rheumatology Review. Springer Nature Switzerland AG; 2020; chap 15. Accessed September 15, 2020. https://doi.org/10.1007/978-3-030-23022-7_15